So much can happen in a week.
Our nation slipped deeper into an abyss of racial division and hatred after the savage, unforgivable killing of George Floyd by four officers in Minneapolis. Protests, the majority of them peaceful, lawful and proper, began and will continue as we try to make sense of all killings of this nature, whether white on black or black on white.
It’s hard to have much hope for our country’s future if so many refuse to have empathy and genuine regard for all human life, no matter our skin color or beliefs. But one need only look at the goodness of people across this great nation during such crises as the COVID-19 pandemic to keep believing there’s a way out.
Or am I only dreaming?
****
I’ve always seen the appendix referred to as a “finger-like appendage.” How perfectly fitting, because it’s an organ that serves no purpose, and when it decides to go kablooey, it actually gives you the middle finger. About 4 inches long, it dangles from the start of the large intestine like a — well, it just hangs there.
We can live without it. It’s a shame it takes something as painful and avoidable as appendicitis — and, worst case, a rupture — for us to end up living without it.
****
The day George Floyd was killed, Memorial Day, I was off work and pretty oblivious to the news. I’d woken up that morning with stomach cramps I’d call bad but not severe. As with other abdominal issues, I figured these would dissipate in a few hours. Our family had eaten Rusty Taco takeout the night before, so I assumed that was the link. I took some Pepto and Imodium (figuring runs were on the way) and napped off and on.
When I awoke mid-afternoon, the cramps were still there. In my haze, I stretched out full-body while still lying down, suddenly feeling an intense pain in my lower right abdomen. What the heck, I thought, did I just pull a muscle? I got up, went into the living room and told Kay, saying, of all things, how could I have pulled a stomach muscle stretching in bed? Or caused a hernia?
So what do we all do when our bodies start doing something weird? We hurry to the internet. I looked up abdominal muscle pulls/strains and hernias but didn’t find much to help me self-diagnose (always a bad choice). The location was definitely out of place for a hernia of any kind, and I felt no bulge, so I nearly ruled that out.
Knowing that Kay had suffered a ruptured appendix 14 years ago, and realizing the location was pretty much where that nonessential organ sits, I decided I’d better look at the possibility. But seeing that appendicitis is rare at my age (59) and that I had none of the other classic symptoms (vomiting, fever, diarrhea), I all but convinced myself that couldn’t be it either.

The pain didn’t really worsen through that evening, but I did a little more research and was befuddled. And I was stuck on the probability that I’d pulled a muscle, for the simple fact that the onset of sharp pain hit at the exact moment I stretched. Looking back, that’s probably when my appendix burst. But neither Kay, who’d been through this before, nor I thought it was my appendix — because of “the customary symptoms” I didn’t have.
Messaging a childhood friend, Alison Lee Shiets, that night on Facebook, I told her what had happened, saying surely I was too old for it to be my appendix. Tuesday morning after a fitful night of trying to find a comfortable sleeping position, I woke up with about the same pain.
I found a 3:44 a.m. message from Alison saying I was NOT too old to have an appendix problem and I’d better get it checked out because if it bursts, it’s serious.
****
I would’ve gone to see my doctor at some point, but may have waited another day if not for Alison (thank you!!!). So I made an appointment with my PCP early that Tues morning for 1:45 in the afternoon. Meanwhile, the pain was worsening and my doc got yelps when he barely touched my appendix area. Sure, he said, it could be a muscle, but it sure presents like appendicitis. So he sent me straight for a CT scan.
After arriving at the imaging place, I sat in the parking lot on the phone wasting time with the insurance company, because our policy insists on pre-authorization for MRIs and CT scans to avoid a $200 penalty. So, silly me, I sat there in my agony and, by the time I was walking inside, I was struggling to do that or stand up straight.

It took a while for them to take me back for the CT because of others ahead of me — plus, they needed me to drink 20 ounces of apple juice, apparently to help improve the scan quality. I asked the staffer at the door admitting patients how long it would be because I was in severe pain, and she said soon. Soon dragged out interminably.
The CT tech had to help me get on and off the table and was above-the-call sympathetic. Because of the possibility of it being my appendix, and with it already being well after 4 p.m., they put a stat on the results.
Just after 5 p.m., while I drove home about 15 minutes after leaving, my cell rang and I hoped it was either the imaging place or my PCP calling. It was the doctor who’d read the scan, and he told me the now not-so-unexpected news: I had acute appendicitis. He’d tried to get someone at my doc’s office to pick up, but they were already closed — and he knew it was urgent enough that he’d better call me directly.
I told him I was almost home and we’d head to the hospital stat.
****
Kay and I couldn’t decide right away whether to dash off to a hospital in Arlington, where we live, or Fort Worth. Knowing we couldn’t waste time, we picked Harris Methodist Fort Worth, where our daughter had been born in 2004. Kay — my angel throughout this ordeal who has taken the best possible care of me, along with all my nurses during two hospital stays — got me to the ER pronto.
She worked to get me past the front-door COVID-19 screener to check-in and triage while a man was telling the screener he had to get in to see a dying relative who’d been attacked in her home. I felt awful for him but was in too much pain to stick around for the outcome.
Kay told the screener I was in an emergency situation and had to be seen ASAP, and as always, she was firm about it. With no visitors allowed, she felt guilty having to abandon me.
Thankfully, my care began almost immediately. An IV was started, morphine given and laparoscopic surgery to remove my appendix set up for that night as I was moved later to pre-op. I met the surgeon and told him I’d heard from staff that he was definitely the man for the job. He said he’d seen my scan results and it was a pretty clear-cut bum appendix.
As I lay waiting for surgery, the nurse taking care of me suddenly said to her colleagues seated nearby, “Did anyone call Dr. (name redacted)?” Apparently she’d been so busy, she hadn’t had a chance to call the surgeon to let him know I was ready for him. So she called, then apologized to me for making me wait quite a bit longer than I needed to. Then she apologized to him when he walked in.
I’m not sure of the time, but I’m pretty surgery started around 10 p.m. By the time I was coming to and could groggily hear a recovery nurse calling Kay to let her know I was out of surgery and would be taken to a room soon, it was well after 11.
I arrived at my room on the second floor of the Harris Tower just before midnight.
****
My general surgeon, a late-40s fellow with salt-and-pepper hair and an easygoing, reassuring bedside manner who clearly likes his patients to understand everything about what’s going to happen and what already has, came to see me around noon the next day. When he told me he’d found not only acute appendicitis but a ruptured, gangrenous appendix with infectious ooze seeping into my abdomen, I couldn’t help myself.
“Shit, it was ruptured?”
Then he showed me the photographic evidence.
I probably should’ve figured on it having burst, based on the severity of the pain, but what do I know about a straight screwy appendix vs. a ruptured one? He assured me he felt confident that he’d gotten all the infection and that I shouldn’t have major problems recovering.
He mentioned the possibility of ileus, a condition that commonly develops with the bowel after abdominal surgery, which can be a serious blockage or involve more of a general disruption of normal digestive function and clear up in a few days. (Side note: According to her death certificate that my birth sister Terry and I located after I found my three siblings, our maternal grandmother, Olive, died of “paralytic ileus” after having a hysterectomy at age 32 in 1934.)
I was discharged early that afternoon, and if I could do it over again, I’d have insisted on staying at least another night. For one thing, I could tell I was dehydrated — and told the doctor and nurses — because my mouth was extremely dry and I was getting cotton mouth just talking. Doc did say that was common with ruptured appendixes (appendices?).
So I clearly needed more IV fluids to get rehydrated, but I didn’t push on that and thought I could rehydrate at home with lots of water and Gatorade. (Was I ever wrong.) It would also seem after surgery for a potentially life-threatening situation, they’d want to keep you longer than 12-13 hours post-op, to make sure you’re *really* OK to leave.
I went home, though, and even though I felt crappy, had no appetite (especially for the clear liquids I had to eat for 2-3 days), felt bloated and my colon didn’t move anything until Friday morning, I knew it was only a matter of time before I started feeling better — especially if I drank those liquids and did nothing but rest. Which I did.
But Friday sucked from the start, from still being dehydrated to vomiting to diarrhea to the horrible way I generally felt. So I told Kay late that afternoon I’d better get to the ER. I’d been in contact with the surgeon’s office earlier about how poorly things were going, and they knew this was a possibility and told me to go if needed.
At the ER, they had trouble drawing blood and getting an IV started, a red flag about my dehydration level. The ER doc came to see me briefly as nurses gave me fluids, anti-nausea med and morphine in my IV and sent me down the hall for another CT scan. A bit later, I went to the bathroom, and when I came back, one of the nurses said I was being readmitted.
It wasn’t long before I was further surprised to see my surgeon walk through the door — I’d figured the ER doc would handle everything. Doc was great and told me what was going on. He said the scan showed I’d developed the ileus he’d told me about, and although he said he didn’t believe it would develop into a serious situation, he and the ER doc consulted and knew I needed to spend time getting IV fluids and meds so I could hold things down and give my digestion a chance to start working itself out.
Soon I was being wheeled across the hospital to the sixth floor of the Richardson Tower. If I’d thought of it at the time and hadn’t felt so dismal, I might have been humming a Howard Jones ’80s song: “Things Can Only Get Better.”
****
The nurses who came to my room looked at the IV in my left elbow, saw my swollen arm around it and said the IV wasn’t working. Apparently it hadn’t taken, or if it did, I was getting little to no benefit.
I’ve always been someone with solid, accessible veins, having donated blood for years after 9/11. But now, I was so dehydrated that finding a “good vein” was proving a tall order for the nurses. A couple tried and failed, and both arms still have the bruising to prove it.
Finally, someone said it was time to call in Kim, the charge nurse that night. It wasn’t long before a not-so-tall, friendly Asian nurse in her 60s came into my room. She looked at my arms and knew she had work to do. She tried another vein on my left arm. Nothing.
Kim then looked at my right bicep area, where I’ve never had blood drawn or an IV placed. I had no idea you could even start an IV there. She started slapping my arm, trying to get the vein to pop up into prominence.
“I’m not trying to beat you up!” Kim said more than once, smiling. I assured her I knew she wasn’t.
She used a heated compress, trying to get the vein of her focus to the surface. She said my veins were rolling and expressed how dehydrated that showed I was.
As Kim worked on that vein for what seemed 20 minutes, telling me not to move, I asked, “Should we pray?”
“Yes, yes, we should pray. Please God, please God …,” she said as I did the same.
Before long, as I refused to look, I asked her if I should.
“Yes! It’s in!”
I told Kim I knew she would come through and thanked her.
****
For the next two days through the weekend, I was cared for by a squadron of nurses whom I could never sufficiently thank for their constant attention and genuine concern for my comfort and condition.
That includes the main nurses as well as the patient care technicians who often took vitals every four hours, changed bedding, logged my info online in my room, brought ice for my water — and, worst of the worst, monitored levels and form (none) of everything coming out of me in the bathroom. I hated having to say, repeatedly, “Sorry, I left some more awful stuff in there for you.”
My vigilant nursing crew started with Vienna and included Chelsea, Nevenka, Sara, Donna, Maria and Kristen. Sara, who’s 45 and only four years ago was early in nursing school, came in twice during the wee-est of hours early Sunday to ask if I needed anything — on a night when I barely slept because of hourly visits from those God-bless-’em nurses.
It was also Sara (not during one of those nighttime visits) who told me her grandmother’s story of her father dying of a ruptured appendix in the late 1920s, when the family lived in the country and there was nothing to be done.
My old memory being what it is, I couldn’t recall today for certain if I’d had an overnight hospital stay before. I’ve had surgeries, but they’ve all been outpatient. I’ve been treated in the ER, but never admitted that Kay and I can recall. Going back to my Texas A&M days in the early ’80s, I do remember stays — one being a few days when I got really sick my freshman year — in the student health center. So there’s that, but since then, I don’t remember any.
This was definitely my first time to experience dragging an IV tower into and out of the bathroom over and over, and up and down the hall for the at-least four walks a day the nurses insisted be taken.
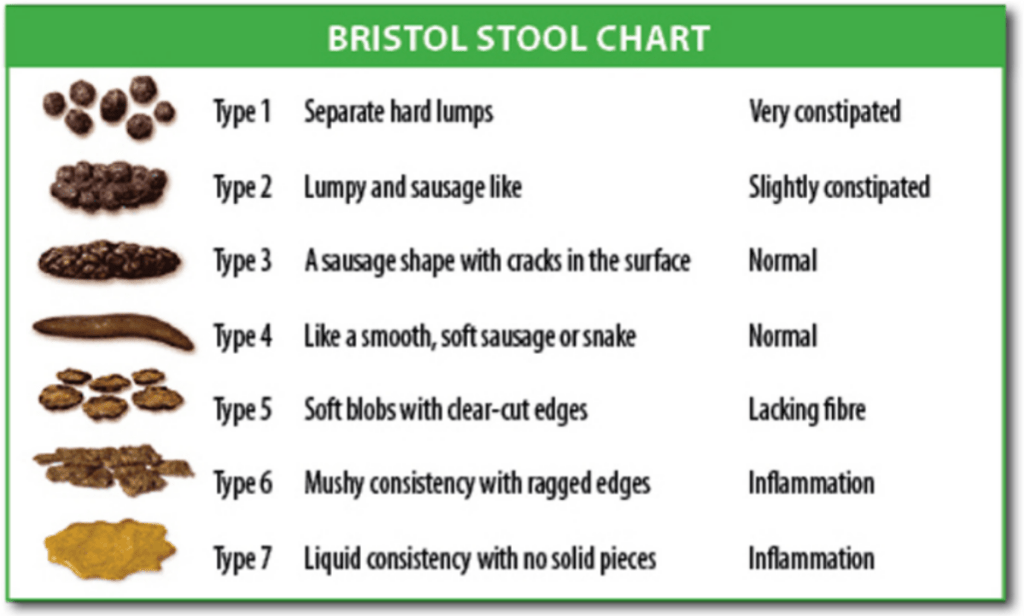
As for the bathroom, I became all too familiar with the Bristol Stool Chart from staring at it each visit, wishing, pleading that I could advance from the bottom (Type 7) up even one notch. Once I asked one of my nurses, “Was that a Type 6?” No, she said almost apologetically. Type 7.
Another memorable component (side effect?) to my hospital stays: getting to experience two COVID-19 swabs. Honestly, they’re not that bad. And although I had to wear a mask in the ER and while taking my walks, patients weren’t required to wear one in their rooms.
****
Since getting home late Sunday afternoon, I’ve made great strides. That night I finally ate some bland solid food — grilled tilapia and rice, courtesy of Chef Kay. In fact, I’ve now had that for five meals, because it feels “safe.” Other than that, it’s been toast, yogurt, applesauce and Gatorade for me. Mmmm!

As for my digestion, it’s still out of whack, but showing signs of coming around. It’ll notch up to Type 6, then drop back to Type 7, then back up again. Dare I hope for Type 5, out of the inflammation/diarrhea range and merely at the “lacking fiber” level? One Bristol Stool Chart baby step at a time.
The surgeon and I will discuss it all at my follow-up Thursday, which we’ll do by phone. We would’ve had the appointment in person, if only my drain were cooperating enough for it to be removed. But I’m still getting out more than 30cc of fluid per 24 hours, and the tube can’t come out until I cross that threshold. I’m making progress, but I figure it’ll be at least early next week.
****
As I continue to heal, Kay and I hope for our nation’s healing to come about, somehow, some way. But so much has to take place for that to happen. *All* Americans have to genuinely *want* to do that, and to *want* the same unity and brotherhood of races. I’m afraid far too many have far too much hatred in their hearts.
Until that changes, we’re just an appendix in a constant state of rupture.
Dear Frank.
Sorry to hear about your appendix! Iâm going to be 60 next week and I think itâs all downhill from there. LOL. I hope you are recovering well.
Best wishes,
Lynn
LikeLiked by 1 person
Hi Lynn! Thank you so much. I’m glad things have gotten better for me this week. I did my first editing shift yesterday…..we’ve been been working remotely for 12 weeks at the DMN! And happy birthday to you! It definitely isn’t all downhill from here! 😊 I hope y’all and the boys have been dealing with all life’s challenges lately. Thanks again and take good care.
LikeLike
Thanks, Frank.Yours too.
LikeLike